![]()
Welcome to the third edition of SurgeXperiences, the first carnival of surgery. I’m honored to bring you this surgical carnival.
This will be a practical and concise edition. The objective of blogs (in my point of view) is to answer questions as quickly as possible, so lets start with the HOW-TOs. Enjoy.
- How to classify fingertip injuries and amputations and how to treat them? This is a nice abstract in where we will learn how to close the wound, maximize sensory return, preserve length, maintain joint function, and achieve a satisfactory cosmetic appearance. This is a Must Read!
- How to survive surgical training when your boss is really mean? A touching and insightful story. Luckyly those times are changing.
- How must be your surgeon? How to make the perioperative experience a smooth one for patients, nurses and surgeons? Great tips for all of us. Don’t lose the floor.
- What are the complications of Mitral Valve Replacement? An excellent reminder.
- How to choose a rehabilitation center? What are their services, facilities, costs and credentials?
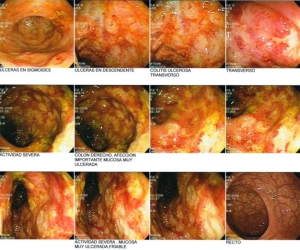
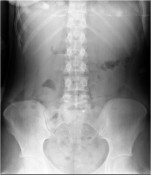
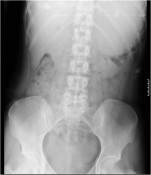
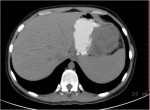
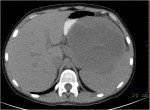
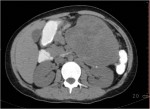
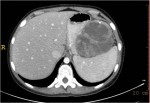
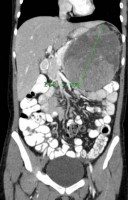
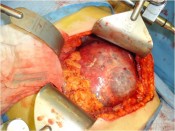
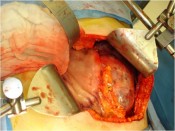
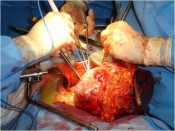
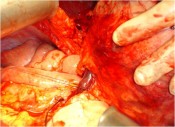
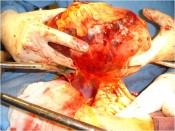
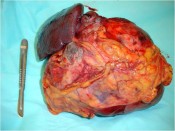
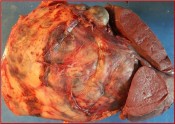
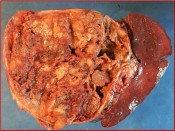
- How is the clinical presentation of severe pancreatitis? I love hard cases as this one.
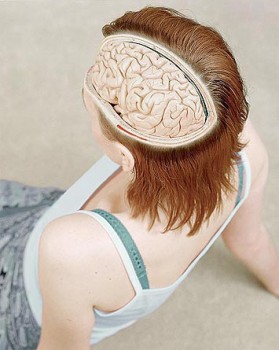
- How much farther have we advanced in medicine since the days of trepanation? Do you know that people had holes drilled in their heads voluntarily and they state that this results in more energy and an increased feeling of consciousness and lessens repression?
- How a prosthetic robotic arm works? Nice videos!
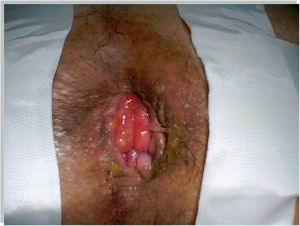
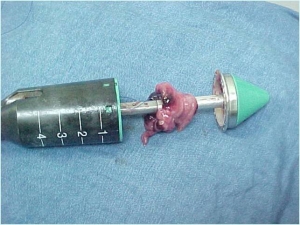
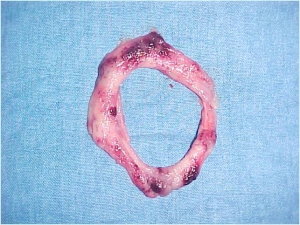
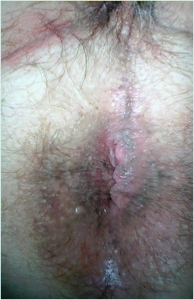
- How a simple procedure (lateral sphicterectomy) can lead to a satisfyingly outcome for both the patient and the surgeon?
- How to interpret the new article that assures the relationship between breast implants and suicide rates?
- How to be thankful to a surgeon and how a surgeon can change your life? Charming story that guides me to always give the best of me.
- How an amebic brain abcess looks like? You will never forget to keep it as a differential.
- How a simple order can trigger a defense mechanism? Try to not give orders to therapydoc.
- Should mesalamine be stopped prior surgery? Why?
- How to manage those the difficult situations involving CPR? A very insightful view and nicely written.
- How to back in time for 3 decades and deny the link between AIDS and VIH? Do you think that the truth may prevail?
- What kind of role a military surgeon play in war zone? Sharing his thoughts and feelings about Air Force training.
Thank you for your time and participation. Make sure you read the next edition of SurgExperiences, created by Jeff Leow